The Precarious Case
Against Precaution
A Deep Dive into the Swedish Cancer Registry
It has been nearly eight years since an expert panel of the International Agency for Research on Cancer (IARC) classified RF radiation as a possible human carcinogen. Since then, neither the World Health Organization (WHO) nor the International Commission on Non-Ionizing Radiation Protection (ICNIRP) has recommended precautionary policies to limit potential health risks.
No U.S. health agency has yet advised the public to reduce RF exposures.
Even after two large animal studies —by the U.S. National Toxicology Program (NTP) and Italy’s Ramazzini Institute— presented clear evidence of a cancer link last year, the WHO has remained silent; ICNIRP responded by calling both animal studies unconvincing.
Now comes the Annual Review of Public Health, which on January 11 posted a paper by five leading epidemiologists who posit that, after a systematic review of all the human studies, they don’t see an elevated cancer risk. The takeaway is that the IARC classification was a mistake.
The two senior authors of the review paper are Martin Röösli of Switzerland’s University of Basel and Maria Feychting of Sweden’s Karolinska Institute. They are both members of ICNIRP; Feychting is its vice chair. A third author, Joachim Schüz, is a senior manager at IARC. The others are Italy’s Susanna Lagorio; and the U.K.’s Minouk Schoemaker.
Though not scheduled to appear in print until May, their paper is at the center of a controversy over whether it was adequately peer reviewed (see Row over Cancer, Cell Phone Review).
One critic, Joel Moskowitz of UC Berkeley, tells me that he believes the authors of the Annual Review paper have “minimized evidence of increased risk” in a number of studies. In what follows, I look at another issue: Whether national cancer statistics —specifically, those in Sweden, can help resolve the brain tumor question.
The Argument Against a Link: Cancer Trends
The 2011 decision by the IARC expert panel was based on epidemiological evidence from the Interphone project and the work of Lennart Hardell, a Swedish oncologist.
One of the review paper’s central arguments is that the IARC decision has to be wrong because national cancer registries do not show a sustained increase in brain tumors years after the widespread adoption of mobile phones.
Röösli and coworkers want us to believe that we can trust the cancer registries. These are “virtually complete,” they write in their abstract. That’s my emphasis and you’ll see why in a moment.
In a slew of papers, Hardell and Michael Carlberg, his collaborating statistician, have reported significantly higher risks of malignant brain tumors (glioma) among long-term (≥10 years) phone users. Both are based in Örebro, Sweden, and are sometimes referred to as the Örebro group.
Since Hardell and Carlberg’s studies were carried out in Sweden, tumor trends there are key to verifying their findings. If their work is right, the review paper maintains, an increase in brain tumor cases should now be detectable in the Swedish Cancer Registry (SCR). “One would expect that any relevant risk should have started to emerge by now,” Röösli, Feychting and the others write.
Many see crosschecking with cancer trend data as a compelling line of argument. Here’s NTP’s John Bucher last spring when he announced that his male rats developed malignant tumors following a lifetime exposure to cell phone radiation: It’s “very reassuring” that there has been “no dramatic increase” in the rate of brain tumors in the U.S., he told NBC News. “It may well be that current cell phone use is safe.” Bucher appears to have more confidence in cancer trend data than his own $30 million animal study.
Is Röösli's team correct that the Örebro results and the cancer registry are out of sync? I decided to take a deep dive into brain tumor trends in Sweden. What I learned is disturbing.
Röösli’s Supplemental Figure 6 Tells a Story
Röösli et al. boil down Hardell and Carlberg’s findings to a single estimate of the brain tumor risk: a 60-70% increase in malignant brain tumor, glioma, after using a mobile phone for ten years or more. If the Örebro group is right, they argue, the SCR should show at least 30% more brain tumors in Sweden.
But the registry doesn’t, Röösli, Feychting, Schüz and the others say, and that means that Hardell and Carlberg must be wrong: There is no cancer risk. Here’s what they wrote:
“Now, in Sweden substantially more than 50% of the population is a long-term [mobile phone] user, and an excess glioma risk on the order of 60-70% would yield an increase of at least 30% in glioma incidence rates, which has not been observed in Swedish people aged <70 years.”
The review paper does not present a graph to illustrate this finding. For that, you have to go to a separate file, posted on the journal’s Web site. There you’ll find Supplemental Figure 6, reproduced below (with some annotation).
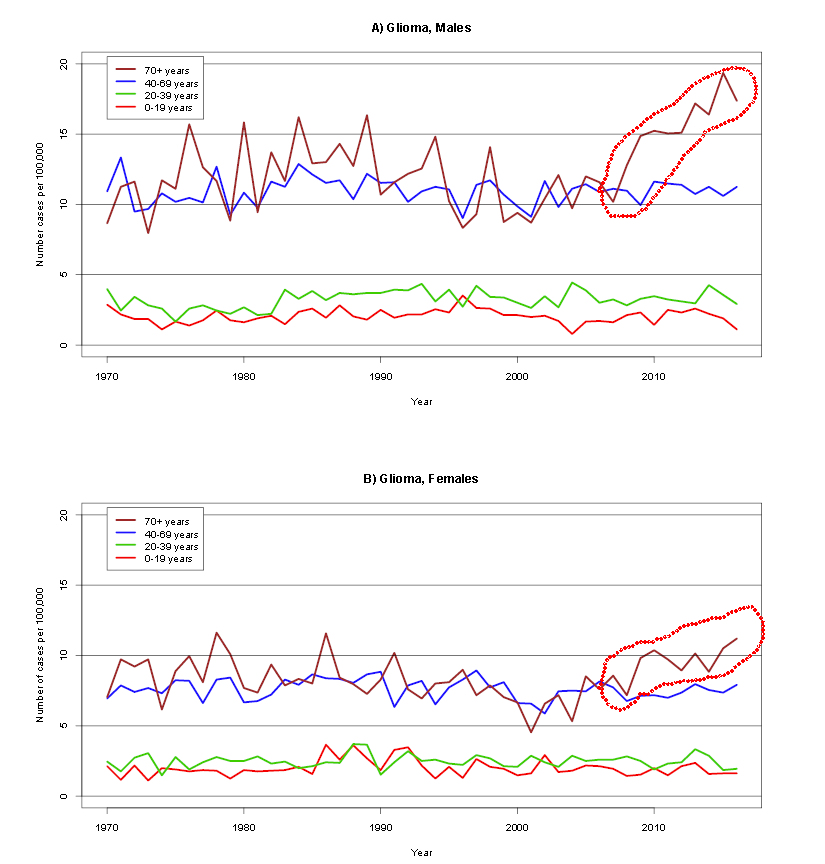
Source: M. Röösli, et al., Supplemental Material, Annual Review of Public Health, 2019
( “...” annotation by Microwave News)
As stated, the graphs do not indicate an increase among those less than 70. They also show that men are more likely to develop glioma than women.
But there is something else about Supplemental Figure 6 that is not addressed in the text: The jump in glioma after about 2005 among men 70 years old or more, and to a lesser extent among the older women (the mauve lines at the top of both graphs). There’s not a word about those jumps.
I asked Röösli why. After all, I wrote, one might expect that those older men to have had the most long-term exposure to cell phone radiation.
Röösli offered what he called “three plausible explanations” for the increase: (1) Cancer registries have long been incomplete for the older age groups, relative to the younger ones. They are now catching up and that accounts for the rise among those ≥70 years old; (2) Better diagnostics, thanks to MRI and CT scans. Tumors that might have been missed in the past are now being detected; and (3) Increase in life expectancy: As fewer people are dying from heart disease, more might develop brain tumors. Röösli added that he is “not convinced” that the older groups had the most cell phone usage.
When I asked Hardell about the jump anong males in Supplemental Figure 6, he replied: “It seems disturbing that they distort the data and just use data selectively to support their no-risk dogma.”
Missing Cases in the Swedish Cancer Registry
In January, at just about the same time that Röösli’s review came out, another paper appeared in the journal Clinical Epidemiology. It shows that the SCR is severely incomplete: Over 20% of all brain tumors treated in Swedish hospitals between 1990 and 2014 are missing from the registry. For malignant tumors, the percentage is a bit smaller, but still more than 18% are not there.
The senior author of the Clinical Epidemiology analysis is Karolinska’s Maria Feychting —one of the five coauthors of the Annual Review paper, which, as I stressed earlier, claims that such registries, presumably including the SCR, are “virtually complete.”
I would have asked Feychting about this discrepancy, but for the last ten years, both she and Anders Ahlbom, her mentor (he too is a coauthor of the Clinical Epidemiology paper), have refused to talk to Microwave News. They cut me off after I reported that they were ignoring a key paper that suggested cell phones are associated with higher rates of cancer. Ahlbom later conceded the error, but the boycott continues.
Instead, I turned to Röösli and asked how he reconciles the two papers. He conceded that this is an “important point.” The underreporting is a particular problem for those over 70 and for benign tumors, he told me. In an email exchange, a statistician at the SCR, Shiva Ayoubi, agreed that these factors are in play.
More than 35% of glioma cases among those ≥70 years old between 2000 and 2009 are not in the SCR, according to the Karolinska’s paper in Clinical Epidemiology. The situation improved somewhat between 2010 and 2014 —but 25% are still missing in that five-year span. That’s one in four. One implication is that the mauve peaks in Supplemental Figure 6 might be even higher if the missing cases of glioma among those ≥70 years old were included. (Because there are fewer omissions in the younger age groups, those changes would be smaller.)
Hardell and Carlberg’s 2015 Warning
There’s an important backstory here that sheds light on the tensions between the Karolinska and Örebro groups.
Back in 2015, Hardell and Carlberg published a paper warning about gaps in the SCR and recommending that the registry be used “with caution” when testing claims about the safety of cell phones. Ahlbom, Feychting and Schüz responded with a letter to the editor, which, when decoded, says that Hardell and Carlberg had misinterpreted the data.
Two years later Hardell and Carlberg followed up with a brain tumor study based on hospital records. When they compared their counts with the brain tumor records in the SCR, the registry came up short. This, they said, proved that they were right.
In the new paper in Clinical Epidemiology, the Karolinska group uses the same type of hospital records —inpatient registers— to check on the SCR. They reach the same general conclusion as the Örebro group. “A large proportion of CNS tumor cases were not reported,” they state.
Feychting and Ahlbom make no mention in this new paper of Hardell and Carlberg’s warnings. I wrote to the first author, Giorgio Tettamanti, an Italian postdoc at the Karolinska Institute of Environmental Medicine, Feychting’s home base, and asked why there is no acknowledgement of, or reference to, Hardell and Carlberg’s earlier work. He didn’t answer.
In a joint statement, Hardell and Carlberg wrote that the Karolinska group’s new paper shows that, “We have been correct the whole time while Ahlbom and Feychting have erred and misinterpreted scientific data, maybe caused by a preconceived no-risk opinion.”
High-Grade vs. Low-Grade Glioma
In the course of the many emails Röösli and I exchanged over a period of weeks, I referred to the paper published last year by Alasdair Philips. He used U.K. registry data to show that those over 60 had developed fewer low-grade glioma and more high-grade glioma: The rate of high-grade tumors (glioblastoma multiforme or GBM), more than doubled between 1995 and 2015, he reported.
Turning back to the Swedish data, I wondered how many of the brain tumors in those mauve peaks in Supplemental Figure 6 were high-grade glioma and how many were low-grade.
Coincidentally, at the same time I was writing to Röösli, a paper appeared by another group of Swedish researchers which addressed this very question.
This new paper, published in Anticancer Research, reports “no evidence” of increased brain tumors in the SCR between 1980 and 2012. The authors note that what they describe as a “relatively stationary” rate of brain tumors occurred during a time of substantial increase in mobile phone use. (The study was financed by the Swedish Radiation Safety Authority to investigate the possible association between phones and brain tumors.)
The Anticancer authors present a graph of the incidence of high-grade (in red) and low-grade (in green) glioma in Sweden in what they label “Figure 1”, reproduced below. (It also gives data for meningioma (in blue), a mostly benign type of brain tumor.)
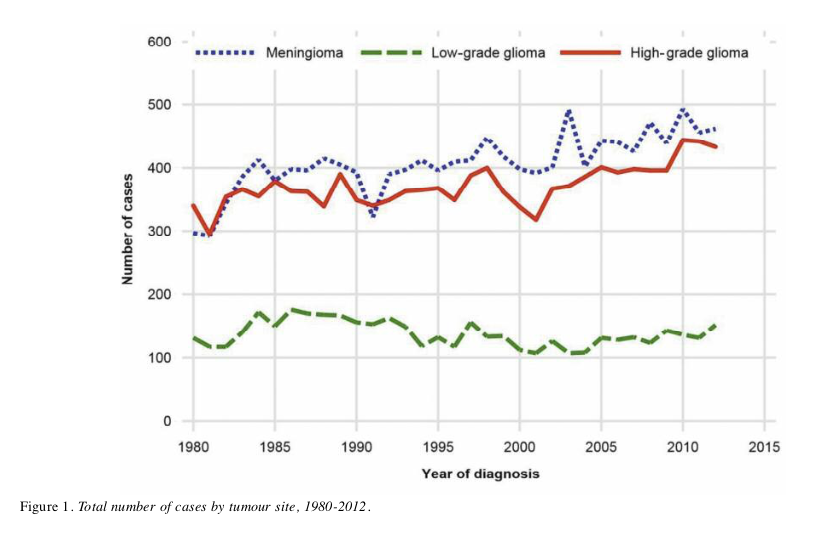 Source: J. Nilsson, et al., Anticancer Research, 2019.
Source: J. Nilsson, et al., Anticancer Research, 2019.
High-grade tumors appear to be following a rising trend since the year 2000. But what is being displayed is the absolute number of cases, which is dependent not only by the size of the population, but also by its age profile. (As you grow older, you are more likely to develop a brain tumor, so one would expect to see more glioma in an older versus younger group.)
The authors go on to present Figure 2, which maps the rate of low-grade tumors and corrects for the changing makeup of the Swedish population. The age-standardized rates show a downward trend. See below.
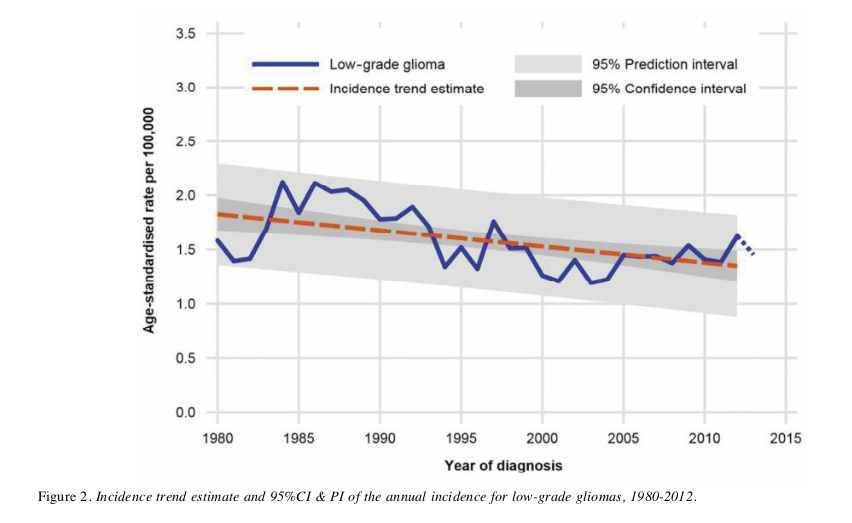 Source: J. Nilsson, et al., Anticancer Research, 2019.
Source: J. Nilsson, et al., Anticancer Research, 2019.
Where is Figure 3: The Trend for High-Grade Glioma?
Strangely, the corresponding figure for high-grade tumors is missing. That is, there is no Figure 3.
I wrote to the senior author of the Anticancer paper, Michael Bergqvist of the hospital in Gävle, north of Stockholm. Why had he not included a graph of the age-adjusted rate of high-grade glioma, which would have been Figure 3? He did not answer. I then wrote to the first author, Jonas Nilsson who works at the same hospital, and asked the same question. He too did not reply.
Like the Karolinska group, Nilsson and Bergqvist used the Swedish Cancer Registry as the source of tumor data, and they too make note of some major gaps. Indeed, their analysis of tumor trends stops in 2012, because, they explain, a delay in registration led to a “misrepresentation of the actual number of tumors” for 2013.
Déjà Vu All Over Again
Figure 2 reminds me of what Alasdair Philips has shown is happening in England: Low-grade glioma are going down while high-grade tumors are going up.
Are GBM on the rise in Sweden too? I wondered. Since the SCR database is available online to all (albeit in Swedish), I asked Philips to chart the Figure 3 that Nilsson and Bergqvist had left out. Here it is:
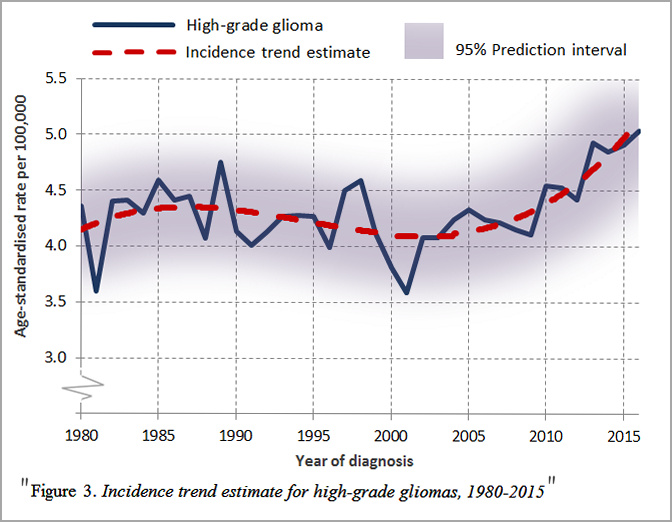 Source: Alasdair Philips for Microwave News
Source: Alasdair Philips for Microwave News
The rate of high-grade tumors has been rising for most of the time since the year 2000.
Philips then took the same data and divided the cases into two groups: those among ≥60 year-olds and those below 60. He plotted the trends for men and women separately:
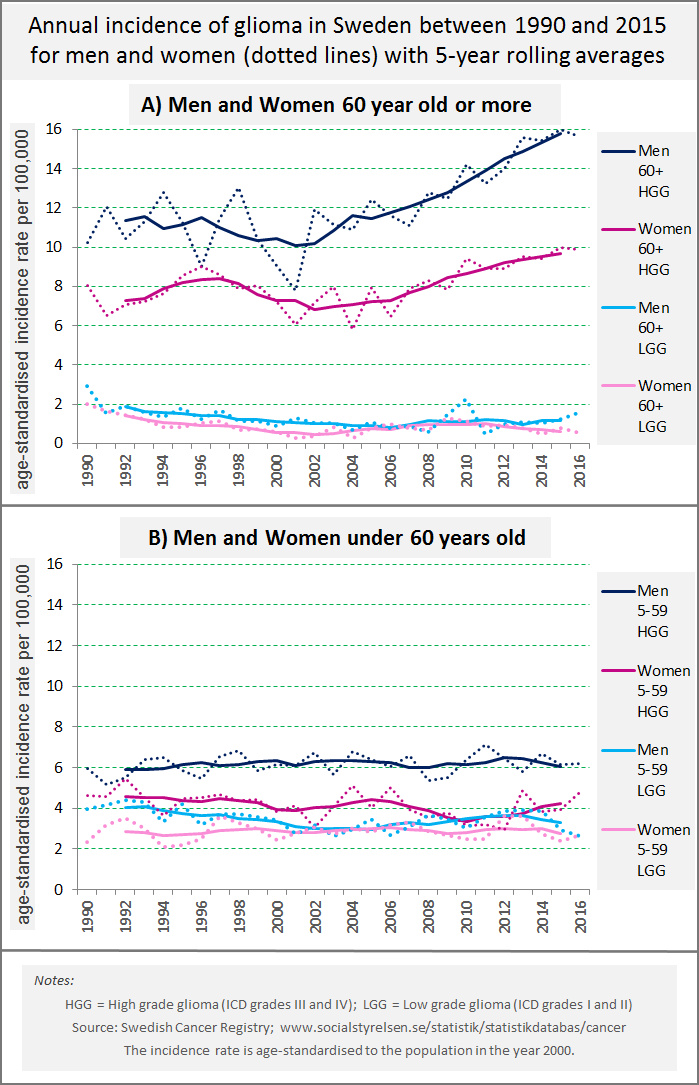 Source: Alasdair Philips for Microwave News
Source: Alasdair Philips for Microwave News
The SCR is incomplete, but these graphs look very much like the trends that Philips is seeing in England, Philips agrees. “This confirms the patterns in the English data,” he said.
I asked both Röösli and Schüz for a comment. In their replies, each made similar arguments. They both discount the changes in the distribution of low-grade and high-grade tumors because definitions have changed over the years.
“Such categorization is very volatile over time,” Röösli wrote. “Every few years new biomarkers are used for coding resulting in different criteria. Thus, you may easily have an increase in some subcategories and a decrease in others.”
“For me, as an epidemiologist, the evidence for brain tumor incidence is very clear,” Röösli concluded, “Rates are stable, in principle, and increase in old people and subcategories can be explained by methodological issues.” (Note: He does not acknowledge the importance of the peak among older males in Supplemental Figure 6.)
Schüz made a similar argument. “Subtype analysis (including by age, sex and location, if available) is useful as long as all subtypes are reported so numbers add up to the totality of brain tumors, otherwise there is a mix between real increases or decreases and shifts between subtypes.”
As for Hardell, he sees it differently: “Of course the type of tumor is most important,” he said.
Who’s right? Is the move from low-grade to high-grade tumors due simply to changes in how tumors are classified over time, or is it possible, as Philips has suggested, that RF radiation is promoting low-grade tumors to a more aggressive and deadly type of brain cancer?
“It needs to be further investigated and possible causes discussed,” Philips recommends.
Precaution or Not?
I am a reporter and editor, not an epidemiologist. As Röösli told me, “Observational epidemiology is sometimes a bit tricky to interpret but [it’s] important to be aware of all the caveats.” I agree, but what I am seeing has so many contradictions and apparent biases that I am left with more than a little skepticism about the no-risk argument advanced in the Annual Review paper.
At one point, I wrote to Röösli and told him, you raise good arguments each time I ask a question, but how can you be so sure when there are so many uncertainties and unknowns: “Do you have any qualms you might be wrong?”
“As a scientist, I try not to think in wrong and right,” Röösli replied, “but let the data speak to make informed and unbiased decisions.”
What do the data tell me? It’s long past time for precaution.
